Program Overview
Get to know who we are, what we do and why we do it.
We do things differently.
Welcome to Call A Doctor Plus, a little company with big dreams of helping our clients save money and improve health, wellness and productivity by putting people back in control of their healthcare.
If you wanted to understand our key philosophies, it would go something like this:
- Healthcare is mess
- Telehealth is awesome
- And it can provide tremendous value to both employers and employees
- But only if people actually use it
- Which is why carrier plans don’t work
- We need to do better for our clients
- And make it easy for them
- And partner with them
- So that they can be wildly successful
If you agree with this philosophy, then you are in the right place.
Keep reading, we’re glad you’re here!
A history of success.
Way back in 2012, which is basically the ice ages in this industry, we stumbled across this concept of Telehealth, which allowed people to connect with doctors and other healthcare professionals over the phone rather than in person and do it on a 24/7 basis in minutes using something as simple as a phone call.
Being brokers by trade, we immediately saw the significant impact that these services could have on our clients, their employees, and ultimately on our business. We realized that by replacing expensive, traditional healthcare with an inexpensive, easy-to-use alternative, we could save our employers time and money while also improving health and wellness.
But we also knew that in order for Telehealth to be successful, people had to actually use it. And the more they used it, the more successful it would be.
So, we set out to build a program that would be easy for our clients to implement and manage, backed by a team to do the heavy lifting and provide hands-on support. We then pioneered the $0 copay plan design coupled with an extensive member engagement plan that would eliminate barriers to use while also driving awareness, adoption and utilization of our services.
6 years later, we’re driving industry leading utilization and delivering unparalleled value to our clients.
How about them apples?
A total telehealth solution.
When the rubber meets the road, most people just want to be happy, healthy and free to live their lives. As a matter of fact, our country was founded on those same principles.
We could not agree more… and you should too!
Recent studies have found that there is a nearly-irrefutable correlation between health and happiness, and that happy employees are 22% more productive than their unhappy counterparts. So, when you improve health, you improve happiness and quality of life, which in turn boosts productivity and enhances the overall state of your clients’ organizations.
This idea is the foundation for what we call our Telehealth Pyramid.
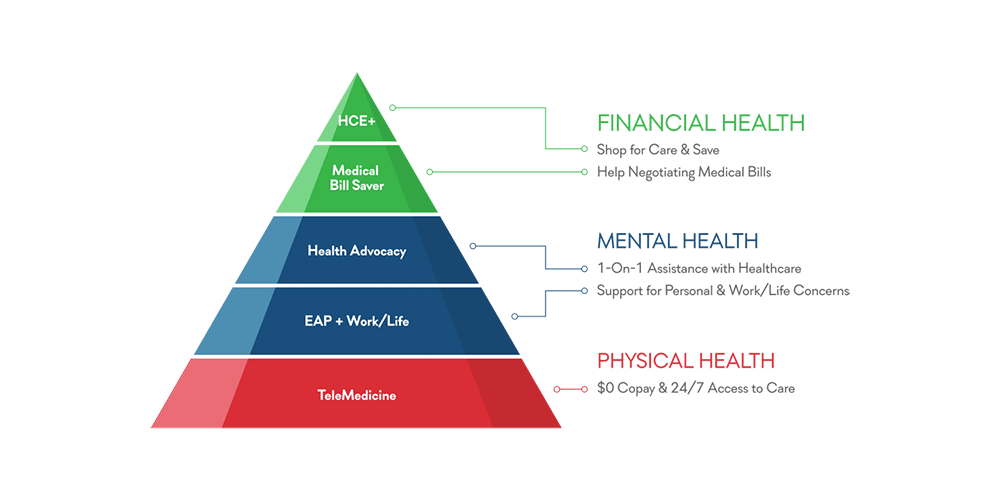
At the core of our offering is Telemedicine, which gives our members 24/7 access to doctors that can answer questions, diagnose common issues and even prescribe medication in minutes.
Unfortunately, this is where the Telehealth offering typically ends for so many plans today, and physician access is all you get. However, our experience shows us that people are dealing with so much more than just their physical health. Many people struggle with a multitude of issues impacting their mental and financial health as well. And just offering Telemedicine alone doesn’t cut it.
This is why our program also provides access to health advocates and counselors, trained to help members with issues that may be causing stress or anxiety, as well as cost saving tools to help address their financial health. By putting all these Telehealth services together, we provide a total pyramid of Telehealth that powerfully impacts health, wellness, financial well-being and ultimately, productivity.
For your body, mind and pocket book.
Utilization drives value.
Checking the Telehealth box isn’t good enough.
Simply offering these high-impact services to our members is insufficient to making a true impact. We need to make sure that people use them. Because we know that the true value of Telehealth comes from utilization. And in our experience over the last 6+ years, we have found that utilization is a product of 4 key ideas.
The first is quality of service. When someone picks up the phone, their experience needs to be second to none. This is why we have selected the very best service providers to include in our plans. We also know that by removing all barriers to entry, like the cost to make a call, program use increases significantly.
In our experience, most of the people we work with have far too much on their plates already, so we have built our program to be easy to implement and administer, and easy for your members to use it. And finally, we need to make sure that members know about these services. What they are. How to access them. Why they will make their lives better.
And this last point is significant to us.
As a matter of fact, our extensive engagement plan uses multiple channels of communication to drive awareness of our programs, which in turn increases adoption, resulting in our industry-leading utilization rates of over 50%.
More use leads to more value.
Who’s on first?
Sometimes, it’s a little confusing as to who does what in our relationship with our clients and their teams. Here is a 50,000 ft. view of who does what.
Call A Doctor Plus – our team helps your clients implement, administer and communicate the programs to their teams. We handle billing your clients, fulfillment of the services, driving awareness, paying commissions and managing our client’s account.
Basically, if it has to do with administering the program, we do it all. When it comes to receiving the benefits, however, that’s a different story and is handled 100% by our partners, Teladoc and Health Advocate.
Teladoc – Teladoc’s team provides your clients’ teams with 24/7 access to doctors by phone, video or mobile app. They are responsible for making sure that the experience our members receive when they need to talk to a doctor is the best it can be.
Health Advocate – Health Advocate’s team of healthcare experts, counselors, social workers and more is responsible for delivering our members with the additional services that we provide, including Health Advocacy, EAP, Medical Bill Saver and the Health Cost Estimator +.
You’ll learn more about these services later.
Delivering significant benefits.
The value of Telehealth is significant, for both the employer and the employee.
For employers, our plan is going to produce happy, healthy employees, which in turn is going to boost productivity and reduce absenteeism. And because the employees have the resources they need to solve their healthcare problems, our plan lessens the burden on your HR team. All this while decreasing healthcare expenses and enabling your managers and supervisors to be as effective as possible.
For members, our program saves money and improves their overall quality of life by giving them easy, affordable access to the quality care they need. By helping members navigate the complex healthcare system and reducing the costs of their healthcare, our program improves health and wellbeing while lowering out of pocket expenses.
What other benefit in your repertoire can check that many boxes and provide such significant benefits to your organization and your team and do it for under $10 a month? The time to engage with these powerful services is now, so put our team to work for you today!
This is the power of Telehealth.
Let us help you succeed!
Our team is committed to partnering with our clients to ensure that they have a successful experience. We do the heavy lifting to make implementing our program easy. We have selected a suite of powerful services that put your members back in control of their healthcare experience.
Our $0 copay plan design and extensive engagement ensures that people know these services are available to them, and that they are using them, which delivers value to your clients’ organizations.
We track and report utilization monthly, so your clients can measure their success and know where they stand. And our proprietary administration system makes managing every aspect of your clients’ account simple.
And when it’s time to pick the plan that works best, there are no extensive forms to complete or start-up fees, you simply execute the agreement, send us their member census and provide a binder check for the first month and you’re on your way!
Doesn’t get much easier than that!
Selling A Case
All of the sales strategies and tactics to close the deal.
We’re obsessed with value.
When someone asks you why they should consider our program versus a competitor, whether it be another telemedicine company, or a carrier plan, the answer is simple.
It’s all about the value, baby!
And we know that value comes from two primary factors…
- Offering a comprehensive suite of Telehealth services to help with physical, mental and financial health
- Creating an environment that makes sure people are using our services.
Everything we do, from the way we built our home-grown administration system to our client success team and how they monitor success to ensure that all our clients are getting the value they deserve… our passion, our goal, our sole obsession is to deliver significant value to our clients and their members.
So, if you want more for your clients then the same ol’ status quo, we are the program for you.
Hey value, here we come!
Getting you up to speed.
Sure, you see the value in Telehealth and how we offer it, but you still have so much to learn in order to effectively sell it to your clients and prospects.
Not to worry, that’s why we’re here!
The best way to get trained on our program is to schedule some time with our sales team where we can review your book, better understand your clients’ goals and plan design, and teach you how to position our program to them, specifically.
If you’d like to connect with our sales team, you can email us or call us at (860) 217-0851 x 2.
If you’d prefer to go it alone, we also have put together a sales training series that you can watch at your leisure.
We’re always here for you!
Get your sale on.
There is no question that the very best sales process is what works for you and your clients. If you have an established book of business, then you already have a proven strategy for how you communicate to them.
If you do have your own process, we can help you integrate our program for maximum success.
If you don’t, here is a flow that might work well for you:
- Send an introduction email to your prospect, linking them to our 2-minute video.
- Make the pitch to your prospect, using our Sales Deck to illustrate the value of our program. If you prefer, you can also invite your prospect to watch the recorded version of our sales pitch, or even sit along and watch with them.
- Send them a proposal of the program, including pricing. For self-funded or larger groups, consider including a Cost Analysis with the proposal.
- Continue to check in with them, asking if they have any specific concerns or objections that you can help them overcome, and consider sending them articles from our Blog to keep our program top of mind.
- Keep at it until they actually tell you ‘no’. Remember, your clients are busy, and Telehealth might not be at the top of their priority list. Don’t assume they are a no; make them tell you.
- If you feel like you are pestering too much and you want to stop reaching out, make sure that you send a final ‘last call’ email, making it clear that this is the last time you will be reaching out. You’d be amazed how many responses this drums up!
And of course, if you want to develop a more customized strategy for your clients, feel free to reach out to our sales team for help.
Happy hunting!
Telling our story.
To help you make an effective pitch of our program, we have created an extensive Pitch Deck consisting of two parts.
Part 1 is our core story. This should take 15 to 20 minutes to present to your client and covers the high-level talking points about our program. Here is our core story in action:
Part 2 is the additional slides. These are more specific slides that are meant to be used only as needed in a presentation. If someone asks for more detail about Teladoc’s doctors, network or prescription practices, or if someone wants to know how we are better than a carrier plan, you can bring them to the relevant slide(s) and walk them through the talking points.
Put our sales deck to use!
World-class partners.
When it comes to the services that we provide to our members, we have partnered with best-in-class service providers in their respective industries. Here is a breakdown of the services provided by our amazing partners.
Overview
Video Link: https://player.vimeo.com/video/104048484
Teladoc
Video Link: https://player.vimeo.com/video/29853062
Core Advocacy
Video Link: https://player.vimeo.com/video/243325538
EAP/Worklife
Video Link: https://player.vimeo.com/video/255395830
Health Cost Estimator +
Video Link: https://player.vimeo.com/video/121497972
This is a good overview of the services that we offer, and you will learn more about how we package and price them in the next section.
It’s all coming together!
A winning combination.
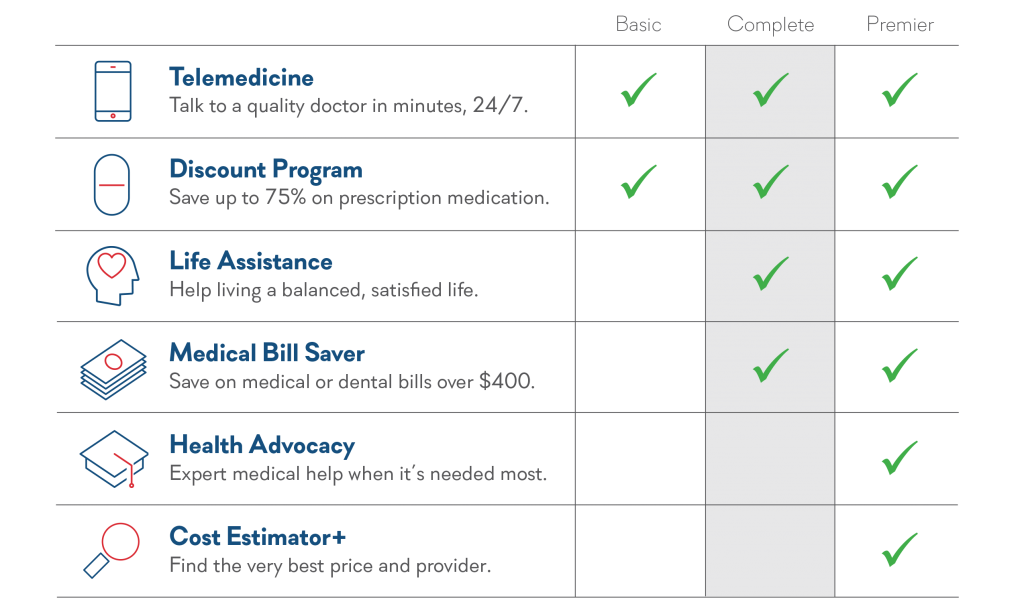
Our plans consist of 3 levels of services, depending on what your clients want, and they are priced based on the size of the group. Here is a breakdown of what is included in each plan, and the standard pricing for each.
If you have questions about our plans & pricing, please contact our sales team and we’d be happy to walk you through it.
Our Plans
Making it official.
Our proposal is a fantastic way to present the program to your client in a personalized, official nature, including pricing for their group. You can use it as a leave-behind, or a good reason to follow-up from your presentation.
And for larger, self-funded clients, we’d suggest including a Cost Analysis for your proposal, so that you can show your clients the ROI they can expect to see by implementing our program.
We think you’ll like what you see!
Get your sale on!
Now that you know about all of the amazing things we do, and how to tell our story, it’s time for you to access all of the awesome sales materials and strategies that we have available for you. We’ll outline much of what is available, but we’re always coming up with more, so check in with our sales team if you have any questions.
And if you need anything we don’t have, let us know and we’d be happy to make it for you!
Video Overviews
- 2-minute overview: https://vimeo.com/104048484
- Program overview: https://vimeo.com/98467200
Sales Sheets
- Healthcare In Your Hands: https://cadrplus.box.com/v/in-your-hands
- Total Care: https://cadrplus.box.com/v/total-care
- Powerful Tool: https://cadrplus.box.com/v/powerful-tool
- Partner In Success: https://cadrplus.box.com/v/partner-in-success
- How It Works: https://cadrplus.box.com/v/how-it-works
- Pick Your Plan: https://cadrplus.box.com/v/pick-your-plan
Service Sheets
- Telemedicine: https://cadrplus.box.com/v/telemedicine
- EAP/Worklife: https://cadrplus.box.com/v/eap-worklife
- Medical Bill Saver: https://cadrplus.box.com/v/medical-bill-saver
- Health Advocacy: https://cadrplus.box.com/v/health-advocacy
- Health Cost Estimator: https://cadrplus.box.com/v/cost-estimator
- Workers Comp: https://cadrplus.box.com/v/workers-comp
Utilization Guarantee
- Broker MOU: https://cadrplus.box.com/v/guarantee-mou
- Agreement Addendum: https://cadrplus.box.com/v/guarantee-addendum
Additional Resources
- HSA Response: https://cadrplus.box.com/v/hsa-response
- I Already Have It Response: https://cadrplus.box.com/v/already-have-it
- Premier Plan Whitepaper: https://cadrplus.box.com/v/beyond-physical-health
- Strategy by Plan Type: https://cadrplus.box.com/v/strategy-by-plan-type
- School Strategy Guide: https://www.cadrplus.com/schools/
- Self-Funded Strategy Guide: https://www.cadrplus.com/self-funding/
- Fully Insured Strategy Guide: https://cadrplus.box.com/v/fully-insured-strategy-guide
- Carrier Plans Sales Sheet: https://cadrplus.box.com/v/carrier-plans
Had enough yet? :)
Enrolling a Case
From agreements to our communication process, it’s all here!
Soup to nuts!
We’ll go into more information about the process for enrolling a new group in more detail through the next few sections, but here is an overview of the entire process in case you’d rather watch it than read it! :)
If you need help with this process, or would like help with your first case, please contact our sales team. We’d be happy to help!!
Keep reading, we have more!
Getting up and running.
Enrolling a new group on our program is easy. There are no extensive forms or sign-up fees. All we require to get the party started is an agreement, member census and first month’s binder check.
That’s it.
Once we have all this information, you can add your groups and their members to our system (or we can help you) and thus begins the process of reaching out to our mutual clients to begin the engagement process.
Here is where you can find everything you need to enroll your next group:
Service Agreements
- Basic: https://cadrplus.box.com/v/sla-basic
- Complete: https://cadrplus.box.com/v/sla-complete
- Premier: https://cadrplus.box.com/v/sla-premier
Member Census
- Census Template: https://cadrplus.box.com/v/member-template
- Uploading Instructions: https://cadrplus.box.com/v/upload-instructions
Payment Information
- ACH Authorization Form: https://cadrplus.box.com/v/ach
- For check payments, mail your check to:
- Call A Doctor Plus
- 35 Nod Road, Suite 102
- Avon, CT 06001
- ACH push payments can be sent to:
- Bank Name: Bank of America
- Name on the account: CADRPlus
- Company ACH Number: 1461682881
- Bank Account Number: 385019300270
- Routing Number: 011900254
That wasn’t so bad, was it?
Let’s get a bit more granular.
The most important thing we need to note about the process is that all new groups needed to be added before the 15th of each month to ensure that they go live the 1st of the following month. If you miss the cutoff, we’ll do the best we can, but cannot guarantee that your group will go live right away.
So, make sure your groups are getting added in a timely manner!
Once you have gathered the required information from your group (agreement, census, binder check), you can then log in to our administration site at https://admin.cadrplus.com, click on the ‘Groups’ tab and then click the ‘Add Group’ link in the upper right hand corner. This page will ask you for some very basic information about the group you are enrolling, like their primary contact, plan and start date. You will also upload the agreement at this point.
After the group is added to the system, we begin our outreach to your new client, in an effort to introduce ourselves to them, make sure we have their correct information, and begin working with them to develop our communication plan.
At the same time, the Teladoc team is setting up your new group for enrollment and making sure that their members will be able to access the system on the 1st of the month. Once all this is done, we add their Teladoc ID to our system, and the member data begins to be sent to Teladoc.
And if you get stuck at any time during the process, our team is ready to help you out!
Have a group ready to enroll, yet?
Help us help you.
If you want to make sure that your group has the best possible experience, you need to remember that the best engagements are a result of what we call our three-legged stool consisting of you, us and your client. In an ideal world, here’s who does what.
What We Do
Our team is at the control center of the process. In additional to being in regular communication with you and your client, we direct the communication process to drive utilization and provide support for anything that you or your client needs. For a more detailed breakdown of our overall engagement process, you can read the next section.
We also review utilization regularly and reach out to low-performing groups to strategize with your client on how we can imrove their utilization.
What You Do
We know you are busy, but we also know that you are looking for good reasons to stay in front of your clients and stay engaged with them. Our most successful brokers use the member information that we provide them to conduct enrollment meetings and make sure that the staff is being told about the program. Of course, we are right there with you every step, but we really see you as the boots on the street.
What Your Group Does
As you will see in the breakdown of our engagement, there is a lot that we can do communicating directly to the member (email, etc). BUT, the most successful clients are the ones that also get engaged in the process. By helping set up enrollment meetings to discuss the program, or using the various tools that we provide them, both initially and throughout the year, they are the true gatekeepers to driving the highest utilization.
When all three parties work together, the results are incredible!
Driving utilization is everything!
Our engagement process is truly what sets us apart. At every step along the way, our goal is to make it easy for your clients to be successful with our program. Here is a breakdown of some of the critical components of our process.
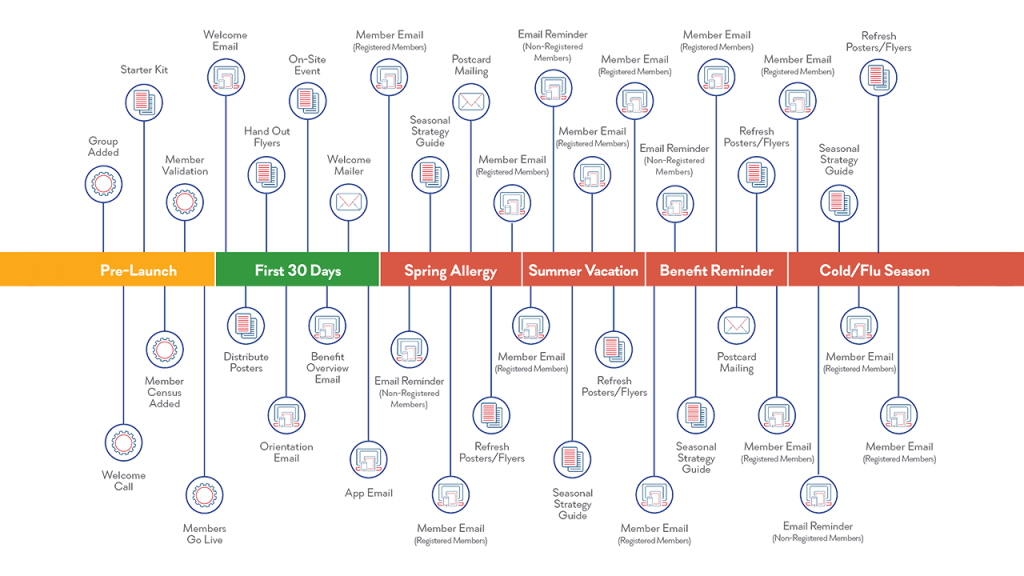
Welcome Kits
For every group over 25 lives, we send out a welcome kit to all new groups containing a flyer, key fob and magnet for each member on the plan. The kit also includes some ideas for how to kickstart the program, as well as a flash drive filled with 12 months’ worth of flyers, buck slips, posters, etc that our clients can use to communicate the program year-round.
Emails
We send a series of 4 emails during the first 30 days of enrollment to all members that have emails in our system. This includes how to access the benefit, why they will love it, and things of that nature. After that, members will receive emails between once a quarter and twice a month depending on whether they have registered or not.
Mailers
There are three mailers that are sent out throughout the year. Welcome mailers with punch cards are sent to all new members about 3 to 4 weeks after they are added to our system. We then send out a postcard mailer to each of our members 2 times a year, once in the Spring, once in the Fall.
Seasonal Strategy Guides
These guides are sent out once a quarter and are appropriate for the current season (Cold/Flu, Allergies, Summer and Holidays). The guides include best practices, as well as links to download the digital materials in order for your groups to further promote the program. The goal of these are to give our clients quick, easy ideas to drive success.
It’s a comprehensive plan, no doubt!
Need More Help?
Our team is standing by ready to get you what you need!
Need Help?
If at any point you need additional help, you can feel free to reach out to our team and we’ll be happy to help. Here are some of the folks who are ready to help!
Broker Support
- Mary Ziko
- P: (860) 217-0851 x 2
- E: brokers@cadrplus.com
Accounts & Member Services
- Alaina Zorzi
- P: (860) 217-0851 x 1
- E: support@cadrplus.com
Accounting & Commissions
- Molly Tebecio
- P: (860) 217-0851 x 3
- E: billing@cadrplus.com

